Spondylolisthesis - Introduction
Spondylolisthesis is where one vertebra slides forward on another.
There are many types including:
There are many types including:
|
It is most common at the low lumbar spine. In can be present without causing any symptoms whatsoever. In fact, about 50% or more of people who have this condition are unaware. It only requires treatment if it is causing symptoms. In the growing child, it is important that if it is detected, they are medically observed to the end of growth.
The degree of forward slippage determines the ‘degree’ of the slip. The amount slippage may be graded as ‘high ‘ grade or ‘low’ grade. Usually, the worse the spondylolisthesis, the more likely that it is to cause pain. This can occur early in life where the bone elongates as a result of a stress fracture, thus usually catching the L5 nerve root where it leaves the spine and causes leg pain (Isthmic Spondylolisthesis). More commonly, degenerative spondylolisthesis occurs with age and affects the nerves contained within the spinal canal (similar to spinal stenosis). Both of these types of spondylolisthesis (Isthmic and Degenerative) can affect both sides of the spine, but occasionally affect one side more than the other. Other spondylolisthesis conditions are rare, including congenital or traumatic cases.
The degree of forward slippage determines the ‘degree’ of the slip. The amount slippage may be graded as ‘high ‘ grade or ‘low’ grade. Usually, the worse the spondylolisthesis, the more likely that it is to cause pain. This can occur early in life where the bone elongates as a result of a stress fracture, thus usually catching the L5 nerve root where it leaves the spine and causes leg pain (Isthmic Spondylolisthesis). More commonly, degenerative spondylolisthesis occurs with age and affects the nerves contained within the spinal canal (similar to spinal stenosis). Both of these types of spondylolisthesis (Isthmic and Degenerative) can affect both sides of the spine, but occasionally affect one side more than the other. Other spondylolisthesis conditions are rare, including congenital or traumatic cases.
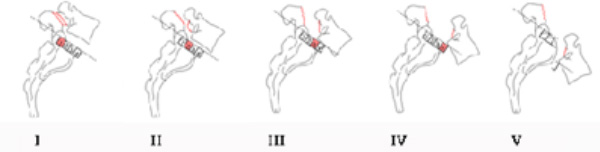
The high grade slippage of grades 3-5 (more often Isthmic) are much less common than grades 1-2 (more often Degenerative or Isthmic).
Degenerative spondylolisthesis is closely related to spinal stenosis and is described separately.
Degenerative spondylolisthesis is closely related to spinal stenosis and is described separately.
Who gets it
Between 4 - 8% of the population will have it. It is sometimes detected as an accidental finding on medical imaging. About half of people with the condition will experience back pain sometimes also causing leg pain. It seems more common in athletes and women. It will sometimes be a cause of back pain in young people.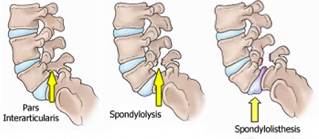
What causes it?
There are differences in frequency of occurrence with regard to gender and ethnic origin, so it is thought to be mainly genetic.
The Patient Line website offers information for patients with spinal conditions:
Sciatica, back pain, spinal stenosis, disc herniation, scoliosis and many other spine conditions explained in a clear reliable, and trustworthy way. Not for profit EUROSPINE experts are here to help patients and their families understand what may be worrying them.
EUROSPINE is a society of spine specialists of various disciplines with a large knowledge of spine pathologies. All well-known and accepted treatment modalities for spine pathologies are represented by the members of the society. However, the Society cannot accept any responsibility for the use of the information provided; the user and their health care professionals must retain responsibility for their health care management.

